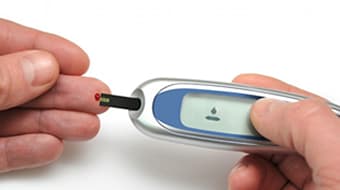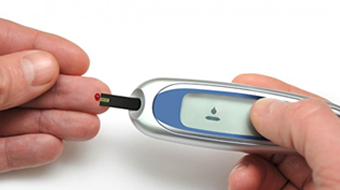
In part one and part two of this series, we discussed different types of diabetes, how you get type 2 diabetes and how type 2 diabetes can cause a host of health issues, some of them life- threatening. We also noted the symptoms and how to diagnose the disease as well as which types of medications are commonly used to treat diabetes. In this final part, we will look at the other means of treating diabetes that can, combined with a proper diet (see a registered dietician who specializes in diabetics), can actually come to cure the disease in many cases.
As far as exercise is concerned it is important to not merely walk. Too many health professionals have made the mistake of telling diabetics that they need only do moderate walking. Walking is helpful but, to achieve the desired results, resistance training is very important and working up to aerobic sessions that have more intensity also brings better results. Here are the current recommendations for diabetics in regard to exercise as stated by exercise physiologist Dr. Len Kravits and his colleague Mathew J. Aquiera:
Resistance Training (muscle building) Recommendations For People With Type 2 Diabetes
- Frequency. At least twice weekly on nonconsecutive days; ideally at least three times a week.
- Intensity. For optimal gains in strength and insulin action, resistance training should be performed at moderate intensity, meaning a lighter weight with more repetitions of the exercise or vigorous intensity-using heavier weights if you are in condition to do so with fewer repetitions.
- Duration. Five to ten exercises performed for the major muscles of the upper/lower body and core with at least 10–15 repetitions performed to near fatigue. In time, the resistance load should increase so you can attain muscular fatigue with 8–10 reps. Three–four sets are recommended for optimal strength gains but even one set has benefit if you truly fatigue your muscles.
- Mode. Resistance machines and/or free weights are appropriate for gains in strength and mass. Optimally, heavier weights or resistance may be required as strength increases.
- Progression. The rate should be slow, to prevent injury. Once the target number of repetitions can consistently be exceeded, resistance can begin to increase.
Aerobic Training Recommendations For People With Type 2 Diabetes
- Frequency. At least 3 days a week with no more than 2 consecutive rest days – Current guidelines recommend five sessions of moderate activity per week.
- Intensity. At least moderate, approximately 40%–60% of maximal aerobic capacity. Brisk walking and other “somewhat hard” exercises usually qualify as moderately intense for most people with type 2 diabetes. Gradual increases in intensity yield more health benefits. Intensity is a better predictor of improved blood glucose control than training volume, so clients should increase intensity before increasing volume.
- Duration. At least 150 minutes per week at moderate intensity or higher. Aerobic activities should last at least 10 minutes and be spread throughout the week. Around 150 minutes per week of moderate-intensity exercise is associated with reduced morbidity and mortality in all populations, though further benefits are likely for those who go beyond the recommended durations.
- Mode. Aerobic exercises that innervate large muscle groups and cause sustained increases in heart rate are likely to be beneficial. Engagement in a variety of aerobic exercises.
(Most of Dr. Kravitz’s research is based on a study in 2010 by Dr. Sherri Colberg and her collegues at Old Diminion University. Dr. Colberg is herself a Type one diabetic and is recognized for her research on using exercise to conquer type 2 diabetes).
Let’s review: The ideal way to live is to lead the kind of lifestyle that will prevent diabetes. This includes eating right, exercising in a balanced way, keeping your stress under control and maintaining an acceptable weight.
If you become pre-diabetic, you can still take control of your situation and reverse these initial symptoms. What full-fledged type 2 diabetics must realize is that they too can turn it all around. With Hashem’s help, the quality of life and length of days can be in your control. And even if your diabetes is advanced, you can still gain a much better quality of life and you can probably reduce your medications enough to make a difference in how you feel.
Your doctor can medicate you and keep you alive and bring a certain level of quality of life for a longer period of time, but he can’t CURE your diabetes. YOU CAN! Just like my client JZ, a 51 year old lady, who became a daily, balanced exerciser, lost 54 kilo (nearly 120 pounds) and got off her insulin and other meds too. Her Endocrinologist pronounced her diabetes-free. It takes hard work, time, effort, patience and commitment, but the benefits you can reap are surely worth this investment. Making the lifestyle changes that are necessary to prevent, cure and improve your diabetes will definitely “add hours to your days, days to your years, and years to your lives.”
Alan Freishtat is an A.C.E. CERTIFIED PERSONAL TRAINER and a BEHAVIORAL CHANGE and WELLNESS COACH with over 19 years of professional experience. Alan is the creator and director of the “10 Weeks to Health” program for weight loss. He is available for private coaching sessions, consultations, assessments and personalized workout programs both in his office and by telephone and skype. Alan also lectures and gives seminars and workshops. He can be reached at 02-651-8502 or 050-555-7175, or by email at alan@alanfitness.com Check out the his web site –www.alanfitness.com US Line: 516-568-5027.
The words of this author reflect his/her own opinions and do not necessarily represent the official position of the Orthodox Union.